Death in Pleasant Valley
Some California prisoners have contracted a cruel and unusual punishment.
Terry J. Allen
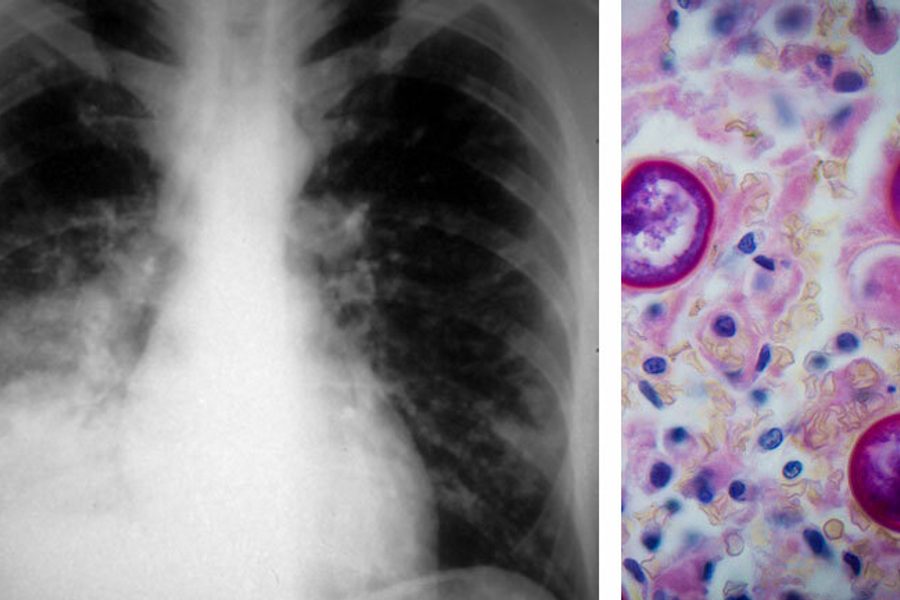
A serious fungal disease you can contract simply by breathing a few spores is 1,001 times more common at California’s Pleasant Valley State Prison than the state average. Non-white inmates are particularly vulnerable.
“Putting prisoners where it is known that susceptibility [can lead] to getting and dying from valley fever … can be the equivalent of a death sentence,” says Warren George, staff attorney with the Berkeley-based Prison Law Office. “And the state has done little.”
Pleasant Valley State Prison (PVSP) and nearby Avenal State Prison (ASP) are at the epicenter of a growing epidemic of coccidioidomycosis, or valley fever. The disease killed, or contributed to the deaths of, 76 inmates at the prisons in a five-year stretch, 71 percent of whom were African-American, according to Clark Kelso, federal receiver for the California prison system.
The reasons why valley fever disproportionately targets these two San Joaquin Valley prisons, and more specifically, their non-white inmates, illuminate the politics of race in America and the fatal consequences of short-sighted healthcare and prison policies.
The disease-causing fungus Coccidioides immitis is endemic to a swath of the U.S. Southwest, Mexico and other pockets in the Western Hemisphere. The spores live quietly in semi-arid soil until disturbed, typically by farming, construction or wind. Although most cases run a flu-like course and disappear undiagnosed, valley fever can be chronic or fatal — especially in high-risk groups.
Once inhaled, the tiny airborne spores can colonize the lungs, clog the respiratory system, travel to the eyes, skin and bones, eat away ribs and vertebrae, and, with fatal results, infect the brain. The disease does not pass between people.
The number of U.S. valley fever infections has skyrocketed to an estimated 150,000 a year. In the last three years, more than 900 Pleasant Valley inmates and 80 staffers have contracted it, and in 2011 alone, PVSP and Avenal reported 535 inmate cases.
The danger, and how to lessen it, has been known for years. A 2007 article on valley fever in the Annals of the New York Academy of Sciences concluded that though the California State Public Health Department had identified preventative measures, “the great majority of these measures were never implemented at any state prison facility.”
Pleasant Valley and Avenal prisons host many of the high-risk factors that turn the disease into a disabling or life-threatening illness. Their large-scale, relatively new construction (1994 and 1987, respectively) in a hyperendemic area disturbed hundreds of acres of dusty, fungus-laden soil.
Another risk factor is a high proportion of non-white inmates. For reasons unknown, valley fever causes more serious and intractable symptoms in blacks, Latinos, Filipinos and some other Asians. Compared with white inmates, the risk of serious symptoms is 90 percent higher for blacks and 30 percent higher for Latinos. For inmates 55 and older, the risk rises to 60 percent.
Healthcare in prison not only mirrors, but magnifies society’s deficiencies and inequities. So it’s not surprising that race also plays a role in the demographics of inmates with compromised immune systems. Tuberculosis, HIV/AIDS and hepatitis C are rife in prisons and further concentrated within some non-white inmate groups. Black prisoners are 3.5 times more likely to have AIDS than white prisoners and comprise 65 percent of AIDS-related prison deaths. Hepatitis C is 10 times more common in prison, and an astounding 80 percent of inmates in some California prisons are infected. Active TB rates among inmates are between 4 and 17 times higher in prison. Both hepatitis C and TB disproportionately affect minorities.
But demographic risk factors aside, prison health services are notoriously, perhaps unconstitutionally, inadequate, and their failure to diagnose early and treat effectively kills inmates.
After reviewing prison reports, John Galgiani, professor of medicine at the University of Arizona, concluded that medical staff at California prisons had sometimes taken up to four months to test for valley fever despite symptoms that should have alerted them sooner.
One 32-year-old African-American inmate, whose case Galgiani reviewed, was sick “for at least two months,” before his valley fever was recognized. He had dropped 15 pounds, was throwing up, had a headache and had been coughing blood. Even after diagnosis the inmate received “inadequate treatment” and developed meningitis, Galgiani testified in U.S. District Court. By then, “it was too late to save him.” With prompt diagnosis and treatment, he added, “this young man might well have survived.”
His testimony was part of a class action that seven current and former inmates who contracted valley fever at Avenal or Pleasant Valley filed in early July against California Gov. Jerry Brown and the Department of Corrections and Rehabilitation. The incarceration of high-risk groups “was the equivalent of conducting a human medical experiment on the inmates, without their consent,” plaintiffs said in the complaint. “While the great percentage of inmates might be expected to survive the disease, for an unacceptable percentage … assignment to these facilities was a potential death sentence.”
Indeed, from January 2012 to January 2013, California prisons saw 18 valley fever-related deaths, says George.
The suit seeks punitive damages and court-supervised medical monitoring for African Americans, people 55 and older, and the immune-compromised, as well as lifetime medical care, including drugs that can cost $2,000 a month.
Despite inmates’ valley fever being largely the result of incarceration, the state washes its hands of victims once they are released. The plaintiffs call the lack of follow-up care an “additional punishment that has been unfairly added to their sentences.”
“Without the medicine, they will die,” their lawyer, Ian Wallach, told the Associated Press. “With the medicine, their quality of life is still unbearable … a life sentence that no judge had ordered.”
On June 24, U.S. District Judge Thelton Henderson had given California a week to start moving some high-risk inmates from PVSP and ASP, and 90 days to complete the transfers. Officials can, however, request an extension. The state pledged to transfer 3,250 immune-compromised and black inmates, but not people older than 55.
Even if high-risk prisoners in valley-fever endemic regions are transferred, remaining inmates will still be at greater risk than the general public.
“My own prejudice about Pleasant Valley, a misnamed place if there ever was [one], is the rate of disease is so high the site ought to be abandoned,” Dr. Royce Johnson, chief of infectious disease at the Kern Medical Center in Bakersfield, Calif., told ABC News. “You cannot tell by looking at someone’s skin color what their risk is.”
Indeed, the disease seems to have an affinity — beyond race — simply for the downtrodden. Valley fever was common during the Dust Bowl, in Japanese internment camps and among migrant farm workers. As such, valley fever is a symptom of a far broader disease infecting America: systemic inequality. The U.S. has today has the globe’s steepest per capita healthcare costs (more than $8,000 per year, though the system ranks 37th in outcome), the world’s highest incarceration rate, and economic priorities that are institutionally skewed against its poorest and darkest inhabitants.
And prisoners are at the bottom of the barrel. The one in 100 Americans who are incarcerated routinely face overcrowding and cutbacks to rehabilitative services, education and training, as well the torture of solitary confinement. Some 30,000 California inmates went on hunger strike this July to protest these conditions.
Adding to that burden is the persistent exposure of some prisoners to a potentially debilitating, life-threatening disease with no vaccine or cure. The practice amounts to “deliberate indifference,” and thus, according to George, violates the Eighth Amendment standard against cruel and unusual punishment.
“If this were a factory, a public university or a hotel — anything except a prison,” said Donald Specter, the executive director of the Prison Law Office, “they would shut these two places down.”









