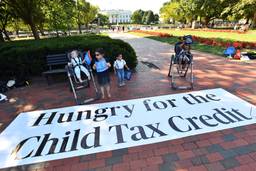During the Pandemic, Poor Areas Have Had Twice the Death Rates of Rich Ones
A new report shows the U.S. response to the Covid pandemic has been defined by inequity—and poor and low-income communities are bearing the fatal cost.
Shailly Gupta Barnes and Jim Pugh

What does equity look like when it comes to governmental pandemic response? As the Covid-19 crisis moves into its third year and the death toll has risen to over one million people in the United States and nearly 15 million worldwide, the question of equity is critical.
An equitable response, first and foremost, prioritizes people who are more at risk and protects them from the worst impacts of the virus. This approach was initially embraced by officials who offered older Americans, people with serious medical conditions, and frontline workers first access to vaccines and booster shots, based on the idea that the most vulnerable deserved protection.
But a recent report from the Poor People’s Campaign highlights a key overlooked demographic in the pandemic response: poor and low-income people. Data from over 3,200 counties across the United States show that, after the first wave of the pandemic, poor counties experienced substantially higher death rates than richer counties. Overall, Covid-19 death rates were twice as high in poorer counties and were as much as five times higher during different phases of the pandemic. This variation in death rates across income groups cannot be fully explained by vaccination status, especially during the later waves of the pandemic: more than half of the population living in these poorest counties had received their second vaccination shots.
To understand the greater risks faced by poor Americans, we should listen to their stories and structure our policy responses around their insights. Denita Jones is a single mom and an essential worker in Dallas, Texas. While Denita received unemployment support early in the pandemic, when Texas ended the lockdown and her place of work reopened in May 2020 she was forced back into a high-risk workplace and lost those benefits. As she described, she was “terrified of going back to work,” but “it’s work or starve, risk my life and the health of my kids or get evicted.”
Marcela Ramirez, a produce packer and undocumented worker in Philadelphia, expressed her frustration with the sacrifices required by low-wage, essential workers. “We are the ones who produce so much wealth in this nation, the ones who could not rest during the pandemic. We are the ones who don’t have the right to get sick, because we cannot miss work.”
Claire Chadwick worked at a big box store in Kansas City during the pandemic. “At first we had no masks,” she said. “The plan for social distancing was chaotic at best, nonexistent at worst. We had lines wrapping around the building and no way to know how many people we had in the store. I worked the front. Then I got the most debilitating headache I’d ever had. Unable to work, I went home. In the county where I live, there weren’t enough [test] kits, so you could only get tested if you were hospitalized. Afraid of those hospital bills, I decided to wait. By the second week, it was hard to breathe. I was so weak I could barely get myself a glass of water. And I wasn’t the only one. Coworkers would just disappear for weeks. We were supposed to be alerted if coworkers tested positive, but since there were so few tests, we often wouldn’t hear anything at all. We’re supposed to get our pay covered if our absence was Covid-19-related, but the lack of testing prevented many diagnoses. Even now, I still experience shortness of breath. My chest gets even tighter when I think of the medical bills to come.” When Claire was finally tested, results showed antibodies that were consistent with contracting Covid-19.
As these testimonies make clear, an equitable response to the pandemic requires more than testing, vaccinations, boosters and treatment. A truly equitable response must seek to provide immunity from what made the virus so devastating to poor and low-income communities. This requires giving poor families enough financial assistance to overcome the added risk factors they face, including the resources and infrastructure required for basic necessities like healthcare, housing, food and water. Nobody should have been forced to risk the safety of themselves and their families by going into unsafe workplaces or deferring critical medical care.
What does this “immunity” look like in practice? The various stimulus programs enacted throughout the pandemic provide concrete examples of policies that alleviated the pressures poor people have been facing. Expanded unemployment insurance provided additional money to a wider population of out-of-work adults through late 2021. While the program struggled with inequities in access, it nonetheless offered substantial support that allowed many low-income families to avoid unsafe working conditions, as Denita’s story demonstrated, and even relieved some individuals of their accumulated debt burdens.
The expanded Child Tax Credit (CTC) provided poor and low-income families with children critical payments every month to cover the cost of necessities, improve their health, and alleviate the emotional and mental pressures of poverty. New research from Children’s Health Watch and the Kairos Center shows that the expanded CTC also reduced hunger and food insecurity. According to the Center on Poverty and Social Policy, the policy also reduced racial inequities among poor children.
While effective, both expanded unemployment insurance and the enhanced CTC have been allowed to expire, with further action stalled in Congress.
In contrast, the Payroll Protection Program (PPP) provided cash assistance to companies, rather than directly to workers, with the aim of keeping people employed. However, it failed by nearly every measure to provide equitable support. According to a 2020 analysis by the Washington Center for Equitable Growth, PPP didn’t reach small businesses in areas hit hardest by the pandemic; it did not encourage businesses to keep workers employed; and it did not effectively reach areas without large financial institutions, which tend to be lower income and include more people of color. The racial disparity of the program was confirmed in a survey of 500 Black and Latinx businesses, which found that only 12 percent received the assistance they requested.
An equitable pandemic response should be informed by these lessons, incorporating programs that ensure sufficient resources actually reach the communities that are struggling the most. As Denita said, “We’re not looking for a handout. We’re looking to survive — not only this pandemic, but in an economy that is rigged against us in the best of times. We need higher wages, better workplace protections, lower rents, access to quality affordable healthcare, and fresh healthy food. Real freedom means not having to choose between your health and your rent.”
The question of health equity is more important than ever, as reports have emerged about a seemingly imminent reversal of Roe v. Wade by the U.S. Supreme Court, which would make abortion fully illegal in many states. While more affluent women may be able to travel to another state where abortion is still legal, poor women who have fewer resources, time, and ability to travel will not have this option. Many will no longer be able to access life-saving medical care. Existing wealth disparities will amplify these unequal outcomes, especially for poor women of color.
What, then, will it take to achieve true health equity for the remainder of the pandemic, and for other health crises in the future? Given the inability or unwillingness among many elected officials to see the fundamental relationship between health and economic well-being, health equity will require meaningful participation by those most impacted by these crises in the political systems where decisions about these issues are made. This means showing up in the streets, voting at the ballot box and organizing relentlessly to translate people power into political power.
Indeed, there are 140 million poor and low-income people in this country. These tens of millions of people account for 40 percent of the country and one-third of the electorate. This represents a powerful political force that could change the direction of our politics and our national priorities. As Rev. Dr. Martin Luther King Jr. said while organizing the 1968 Poor People’s Campaign, “There are millions of poor people in this country…if they can be helped to take action together, they will do so with a freedom and a power that will be a new and unsettling force in our complacent national life.”
The Covid-19 pandemic has cost the United States, and the world, greatly in lives lost. Through this painful process, we’ve learned important lessons on what does, and doesn’t, protect people during a health crisis. It is now time to apply those lessons and bring those who are at the margins of our politics and policy-making to the center.
Shailly Gupta Barnes is the Policy Director at the Kairos Center.