The COVID Public Health Emergency Declaration Has Ended. The Emergency Isn't Going Anywhere.
1,200 days in, the public health emergency comes to an end. Can the Left fight back?
Update: The national public health emergency declaration for COVID-19 will expire at the end of the day on May 11, 2023. Some 150 people in the United States continue to die of COVID-19 every day.
In this year’s State of the Union address, President Joe Biden took care to portray the ongoing coronavirus pandemic as a trial that is behind us and a victory for the people. “Today, Covid no longer controls our lives,” Biden said, adding that “while the virus is not gone, thanks to the resilience of the American people … we have broken Covid’s grip on us … And soon we’ll end the public health emergency.”
This rosy depiction belies reality. Even by the official count, hundreds of people in the United States are dying of Covid-19 daily. In recent months, more than half of all Covid deaths have been among people who are fully vaccinated. Millions more are experiencing the disabling effects of long Covid, a condition our systems of healthcare and social welfare have struggled to appropriately address. The official policy for medically vulnerable populations, the disabled, the immunocompromised and older people is that they politely remove themselves from society — “back to normal” is not intended for them.
The Biden administration has been chiefly responsible for normalizing this ongoing tragedy, and that work is set to culminate this spring. On May 11, the Biden administration will end the official designation of Covid as a public health emergency, just 1,200 days after it was first declared on Jan. 27, 2020. This act will close the state’s assumed primary responsibility for the pandemic and its effects and herald the beginning of the next era of Covid, one where the private market rules the pandemic response.
In effect, the Biden administration is throwing Covid to the maw of the U.S. private insurance market, shifting both the payer and the responsibility to our predatory and extractive for-profit healthcare system. Costs will rise, the uninsured and underinsured will face tough economic choices, and pandemic-related resources will be stratified and rationed by a person’s ability to pay (like all other U.S. healthcare).
As these first 1,200 days of the pandemic come to a close, the federal government is relieving itself of responsibility for the ongoing death, disability and debility wrought by Covid at a time when continued intervention is critical. To get the next 1,200 days right, we need to understand that the story of Covid has been a story of class war.
And despite our many losses, it’s one we can still win.

In early 2020, a very different pandemic response was possible in the United States. Faced with the combined existential threats of a Trump presidency and a novel pathogen, we saw mutual aid projects and strikes over Covid protections proliferate. Prison abolitionists pressured state and local governments to “Free Them All for Public Health,” demanding the emptying of jails and prisons. Mutual aid networks delivered food and medicine to disabled people and elders and worked to keep people from being evicted.
That brief moment exposed the many fictions meant to excuse everyday austerity conditions in the United States. In a rush to curtail the disastrous effects of mass unemployment, the federal government added hundreds of dollars per week to the average unemployment insurance payment, in addition to making direct stimulus payments to individuals — without means testing. Under pressure from activists, the federal government also pursued eviction moratoria, even if the implementation was deeply insufficient and flawed. Student debt payments were frozen. Supplemental Nutrition Assistance Program funding and eligibility increased. Medicaid funding and eligibility also increased, with a new provision ensuring that individuals could not be kicked off Medicaid rolls until the conclusion of the public health emergency. A fund was created to pay for Covid treatment, including hospitalization, for people without health insurance.
Each of these measures was the kind of enhancement to the U.S. welfare state that we are routinely told there is simply not enough money for.
By late 2020, however, much of that early Covid response focused on welfare supports and non-pharmaceutical interventions began to fade, a process that accelerated after Biden came into office. For all its promises to “follow the science,” the Biden administration’s Covid doctrine has been one of personal responsibility and individuated risk, and the trajectory of the Biden pandemic response is best understood as the systematic dismantling of protections, including the few worker protections that Biden initially promised during his campaign.
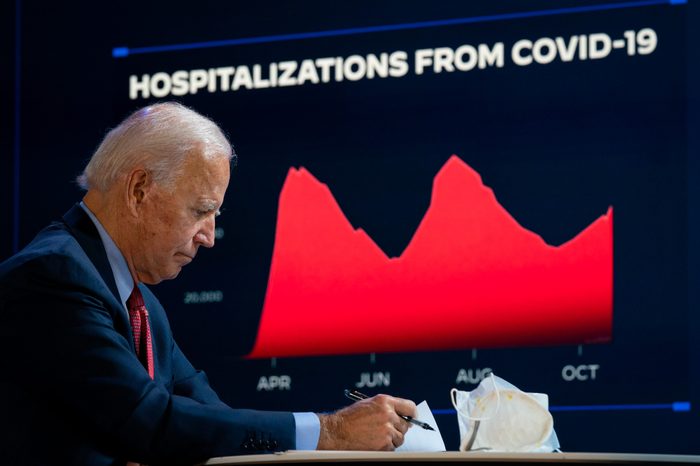
Shortly before the 2020 election, Biden made it clear that his priority was protecting the capitalist economy at the expense of lives. He pledged that ideas like paying people to stay home were not going to happen, saying, “I’m not going to shut down the economy. I’m going to shut down the virus.” The Biden transition team was similarly quick to walk back the idea of a four-to-six-week shutdown to drive down the virus’ spread after it was mentioned by a Biden adviser in an interview with Yahoo Finance. In a round of press appearances, Biden advisers denied the incoming administration would do such a thing, with soon to be Surgeon General Vivek Murthy telling Good Morning America, “We’re not in a place where we’re saying shut the whole country down. We got to be more targeted.”
Once in office, Biden made his agenda even more clear. Jeff Zients, the man named as lead strategist of Biden’s pandemic response, was not a doctor or a professional in public health or health policy. Instead, he was brought in straight from the world of private equity to lead a push to reopen businesses and schools. Zients took on the pandemic response with a mantra that demonstrated his total obliviousness to symbolism: “Execute, execute, execute,” reportedly uttering the word so frequently that aides had it stitched into a blanket.
Under Zients, Biden’s policy pivoted even farther from collective responsibility and welfare-based interventions.
After famously promising another round of $2,000 stimulus checks, for example, the administration only sent out $1,400 checks, claiming an earlier round of $600 checks made up the difference. Other campaign trail promises never materialized at all, including a 100,000-strong national contact-tracing workforce, “rigorous” new Covid-specific guidelines from the Occupational Safety and Health Administration to protect workers, and federally guaranteed paid sick leave for anyone sick with Covid (or caring for someone who is).

The administration also oversaw the dismantling or premature end of pandemic-era welfare expansions, fleeing as many associations with these programs as possible. As expanded unemployment came to an end, the Biden administration didn’t fight to keep it, with unofficial White House adviser Larry Summers — whom aides reportedly nicknamed the “shadow director” of the National Economic Council — later erroneously pointing to the program as the main driver of inflation. After a brief expansion of testing infrastructure, the administration scuttled most federally financed testing, and by early 2022, it became almost impossible to truly know how much Covid transmission was even happening. In December 2021, the Biden administration shortened its recommended Covid isolation time from 10 days to just five. This decision wasn’t based on new information about the duration of the average Covid infection (which can often last longer than 10 days), but instead, in Anthony Fauci’s words, because there was a “danger that there will be so many people who are being isolated [at one time] … that you could have a major negative impact on our ability to keep society running.” The effect was to keep workers at work, even through illness, at the cost of their health and lives.
Reduced spending on testing and a shortened Covid isolation time came despite some within the Centers for Disease Control and Prevention (CDC) raising the alarm about the ongoing pandemic. An internal CDC slide presentation leaked in summer 2021 acknowledged breakthrough cases were happening; one slide included an appeal to the Biden administration to recognize that “the war has changed.” But when presented with real-world evidence that its actions were not controlling the pandemic and might even be exacerbating its effects, the Biden administration stayed the course, never learning from its mistakes.
Most egregiously, the Biden administration spearheaded the mass abandonment (and even stigmatization) of universal masking, still one of the most important pandemic interventions we have. Shortly before entering office, Biden told Jake Tapper that, upon inauguration, he would ask the people for just 100 more days of masking — “Just 100 days to mask, not forever.” The Biden administration stuck to this promise despite ongoing Covid deaths and CDC evidence documenting breakthrough infections. In a rush to declare “independence from the virus” by Independence Day, the CDC issued a dramatic reduction in masking recommendations May 13, 2021 — 113 days into Biden’s presidency and just 473 days into the public health emergency. Prior to the CDC’s announcement, roughly half of all U.S. states had indoor mask mandates in place. Of those states, at least 20 dropped their mask mandates shortly after the CDC’s announcement, many specifically citing CDC guidance. By July 27, when the CDC reissued masking recommendations — a seeming acknowledgement that their guideline change had been premature — the damage had been done. Only a handful of statewide mask mandates remained across the country, and 15 of the 20 states that allowed mask mandates to expire in spring 2021 have never seen them return. The remaining states dropped their mask mandates by early 2022.

Now the vaccines, long the nearly exclusive focus of the federal pandemic response, are set to be passed to the private market. Once the federal supply of vaccines runs out, uninsured people (and insured people who get the vaccine from an out-of-network provider) will face out-of-pocket payments or copays to get vaccinated and boosted. While the Biden administration has pledged to maintain free vaccination for the uninsured, the details of the plan remain vague. As we come to the end of the first 1,200 days of Covid, the federal government is in such a rush to return things to “normal” that even vaccination is not something it can acknowledge as a universal good.
Beyond vaccination, the outlook is worse. Treatments like Paxlovid — a centerpiece of the past year of federal intervention — will be fully privatized and their cost left to insurance companies to determine. Covid testing will also be left to insurance company discretion, further hindering many from seeking treatment while obscuring an already miserably opaque picture of Covid’s ongoing spread. Medicaid expansion ends April 1, bringing with it a wave of eligibility redetermination that will see up to 15 million people lose health insurance.
And yet, as the federal response comes to an end, the pandemic remains unflinching, meaning the first 1,200 days of Covid may soon become a substantive outlier in the broader trajectory of the pandemic.
Alongside the unwinding of pandemic policies, the Biden administration has gone to significant lengths to portray the pandemic as primarily a concern for a small fraction of the population. In 2021, a common refrain for officials was “a pandemic of the unvaccinated,” a position Democratic Gov. Jared Polis summarized by saying, “If you have been fully vaccinated, the pandemic is largely over for you” in a statement announcing the end of a mask mandate in Colorado. Despite data showing that as many as 60% of Covid deaths in a given month are among the vaccinated, in October 2022 Biden stated that “almost everyone who will die from Covid this year will not be up to date on their shots, or they will not have taken Paxlovid when they got sick.” Similarly, in early 2022, in an interview with Good Morning America, CDC Director Rochelle Walensky said it was “encouraging news” that the majority of people dying of Covid now had underlying conditions and were “unwell to begin with,” a statement that, in addition to devaluing the lives of disabled and immunocompromised people, had no sound evidentiary basis.
The effect of these positions was to paint the ongoingness of Covid as something happening to other people. This form of cruel optimism — shared by liberals and conservatives alike — sought to solidify the idea that the only people dying of Covid were already close to death or were personally responsible for their illness.
In this way, the Biden administration’s pandemic response has placed renewed emphasis on the tenuous, imaginary line that lies between the healthy body and the medically vulnerable body.

Our collective understanding of our relationship to this new virus has been pummeled with fantasies about understanding our own individual risk and acting accordingly. The previous, more solidaristic framings of the pandemic — like the once-common refrain, “my mask protects you, your mask protects me” — have slowly eroded, replaced with a slurry of advice about weighing individual costs and benefits based on whether one has pre-existing conditions. This rhetoric of individuated risk has inspired many to feel assured of their own health at the expense of the health of others.
In our book, Health Communism, we show how state policies shape and emphasize these distinctions between the healthy body and the medically vulnerable body in defense of the status quo, a dynamic on full display in the Covid response.
Fantasies of one’s intrinsic health mean little to those with long Covid, including those we’ve spoken to in the past year who developed the condition despite being, in Biden’s words, “up to date with their shots.” Many have told us that the experience entirely upended their understanding of their bodies and that, prior to their Covid infection, they would have thought of themselves as archetypally “healthy” individuals, a binary they now question. Even more people have told us they now feel more alienated at work than ever, forced by supervisors to work unmasked or risk losing their jobs. When they inevitably get sick, in addition to the risks inherent to the illness itself, they lose shifts and wages, and it throws their home life into chaos as they struggle to keep their families or roommates from becoming ill. Some have described this as feeling like a constant cycle they can no longer imagine ending.
These accounts reflect a reality the Biden administration has failed to understand. There is no individuated escape from the pandemic. There is no “targeted intervention” that will end it for some but not all. A pandemic is an inherently relational phenomenon, and transmission is a social process. The rhetoric and policy of personal responsibility and individuated risk has been literalized on us by force. To counter it, we will need to take aim at the state.
As we near the conclusion of the pandemic’s first 1,200 days, organizing toward a more collective pandemic response is set to become even more difficult. With responsibility for public health and the ongoing pandemic increasingly shifted off of the state and onto the private market, the number of actors we will have to target for demands will be increasingly dispersed. Federal, state and local governments will have a renewed list of private actors on whom to deflect blame: health insurance companies, pharmacy chains, hospital groups, pharmaceutical companies and employers. All these entities are powerful — and widely loathed — stakeholders in U.S. political life, but the scope of their power is shaped by the state. The current plans to privatize Covid care amount to an expansion of the power of those groups.
We have been on this trajectory of fragmentation for some time. Many of us have gotten so used to being on the back foot in Covid advocacy that it can become difficult to imagine otherwise. Where once it was common to see demands, even from centrist and moderate public health professionals, that we “pay people to stay home,” many have dropped that assertion, wary of its association with an economic “shutdown” (itself a demand many of us once embraced). Many in public health have altogether dropped the term “mask mandate,” preferring to politely ask that the CDC universally “recommend” masking. Soon, when once the federal government was the central target for us to pressure to expand its paltry vaccination efforts, we will instead be caught up demanding Pfizer reduce the price of its vaccine, or of Paxlovid, on the private market. Organizers in individual states will likely have to press their state governments to expand access to Covid testing, vaccines and treatments under Medicaid. And so much activity, both for Covid and its longer-term impacts in long Covid, may slowly mold itself in the image of the abysmal charity-industrial complex model that permeates and compromises so much disease-based advocacy work in the United States.

We share this bleak assessment of a possible future not to demobilize, but to agitate. As we come to the conclusion of these 1,200 days, we will have to make demands that go far beyond many of the platitudes that have become mainstays of pandemic-era discourse. It is not enough to say we must “follow the science” in hopes that some putatively unadulterated truth will sway what are nakedly political and economic decisions. It is not enough to wish for soul-searching within the discipline of public health because public health does not, in and of itself, outlay a program for political action; it merely gives us a set of tools and operations with which to understand the world.
To build a better future together, we will have to commit to setting aside the false binary between the “healthy” and the medically vulnerable that many of us carry even into spaces of radical and anticapitalist work, and instead acknowledge our collective vulnerability.
A commitment to making our organizing spaces safe, even for the most vulnerable, is also a commitment to making those spaces safe for everyone. On a recent episode of our Death Panel podcast, Kelly Hayes, an organizer with the Lifted Voices Collective and co-author, with Mariame Kaba, of the forthcoming book, Let This Radicalize You: Organizing and the Revolution of Reciprocal Care, emphasized: “Lack of consensus around Covid safety, lack of regard for the well-being [of] disabled people … has been extremely harmful to our movements.” Hayes added, “The world has changed. And that’s very hard … [But] the process of accepting that ‘this group is now expendable’ or ‘that group is now expendable’ is how they will destroy us all if we allow it.”
These measures can help us to build movements powerful enough to make demands on the state, beginning with the restoration of pandemic interventions the federal government once pursued but has since abandoned. The federal government should pressure state and local governments to issue mask mandates, especially during waves, and should provide free masks. Covid vaccines and therapeutics must not be consigned to the private market; they must remain free to all. Moreover, the vaccine rollout itself needs to be expanded, whether through pop-up clinics or programs going door to door. Covid care and hospitalization should be paid for by the federal government again. Testing infrastructure should be reinstated. A federal sick leave guarantee should be created — not just for Covid but for all sickness. The federal government should finally issue OSHA guidelines that apply across sectors and establish a high standard of workplace safety. Title 42, the xenophobic Trump-era border policy enacted in the name of the pandemic (which the Biden administration embraced) must not be replaced with an equally horrific policy. The list goes on.
If the federal government wants to consign us to a perpetual Covid crisis, we must demand that, at minimum, they continue to be responsible for guiding the response and paying for mitigations, testing and treatment.

In the longer term, we must demand not only Covid mitigation but a response to the deep inequities in our broader political economy that predate Covid. One of these demands is for single-payer healthcare, or Medicare for All. The privatization of Covid care, and several of the issues highlighted above, would not be as profound an issue under a system that guaranteed all care for all people. Another is housing and food guarantees, so people aren’t forced to return to work sick simply to afford food or shelter. We must enact prison abolition, as it has never stopped being true that it’s necessary to “free them all for public health.” Our social welfare programs must be expanded and the barriers to qualify for them not only lowered but made less onerous; individuals on disability programs, like Supplemental Security Income or Social Security Disability Insurance, as well as seniors on Social Security, need substantial increases in economic supports so they aren’t forced to live in poverty. Long-term care in the United States needs to be reworked entirely, making it possible for people to live in the community with guaranteed shelter, rather than in nursing homes that have been a locus of Covid transmission and deaths from the very beginning.
This list of broader demands may seem fantastical, but these are not loose ambitions. They are simple, if transformative, changes to our political economy. And this is a moment that requires transformative action toward a larger horizon of bringing a final end to capitalism.
Crises like Covid are best understood as political crises, shaped by what Friedrich Engels called “social murder,” the process by which the state makes certain populations more susceptible to premature death and maiming. Our colleague Nate Holdren, a legal historian of capitalism at Drake University, argues in a forthcoming work that this process of social murder is endemic to capitalist political economies and that we cannot end social murder without ending capitalism. “The capitalist state tends to redistribute rather than to end mass killing,” Holdren writes. “In doing so, the state tends to encourage opposition to social murder to become fragmented.”
We believe we are in such a moment of contestation. Having prioritized capital over lives, the state is intent upon relinquishing its responsibility for Covid, dispersing our attentions to the litany of private and public actors that make up our miserable healthcare system. While the pandemic has been long and brutal and taken so much from so many of us, its effects (especially in the forms of organized abandonment and of social murder) have only just begun, if we keep to our current trajectory.

Yet we must not despair at what was not achieved in these first 1,200 days. The history of social movements is not a neat and linear path, and the early years of an ongoing crisis do not have to define how subsequent years play out. ACT UP, the radical group that fought social murder at the height of the HIV/AIDS epidemic, only emerged several years after the crisis began. “What I really needed to hear when Covid protections started to be ripped away in 2022 was that it’s not too late,” organizer Alex M. (whose full name is withheld due to the nature of their organizing) told us on a recent episode of Death Panel. “Just because we’re three years or more into a pandemic does not mean that it’s too late to start organizing, or join organizing around the pandemic.”
Covid cannot be neatly compared to past crises, but that is not to say it is unique. We are enmeshed in a historically specific and politically contingent example that happens to underscore how movements for disability justice, abolition, health justice and economic justice are, and must be, connected to each other and (broadly) to movements against capitalism.
As we come to the conclusion of the pandemic’s first 1,200 days and face increased state abandonment, it’s vital to remember that it’s not too late to get the next 1,200 days right.