At Angola Prison, Getting Sick Can Be a Death Sentence
A 6-month investigation into the largest maximum-security state prison in the country.
Katie Rose Quandt and James Ridgeway
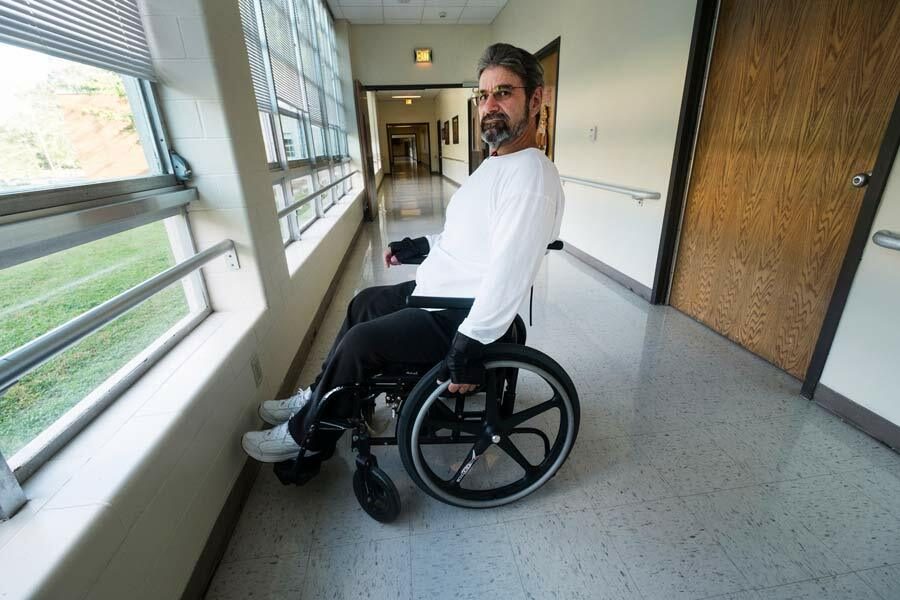
ON A HOT DAY THIS AUGUST, Francis Brauner, 51, wheels his chair through the halls of the Villa Feliciana Medical Complex, a state-run nursing facility in Jackson, La. Love bugs, clinging together in pairs, swarm on the complex’s low-slung brick buildings. Brauner has just learned his protein levels are too low to proceed with the surgery scheduled for the following week, and he is trying to come to terms with his disappointment.
Brauner, imprisoned on a rape conviction he maintains was wrongful, had his life change forever in 2005 when, working in the fields at Dixon Correctional Institute, he suffered a back injury that left him paralyzed from the waist down.
Brauner was transferred from Dixon to Louisiana State Penitentiary, better known as Angola. Classified by an officer as dangerous — despite being unable to walk — Brauner was placed on a bed in solitary confinement, without access to a wheelchair. The pressure of his own body wore on his skin and created bedsores, which became infected. The infection tunneled through his buttocks and scrotum, exposing bone. Within a month, it reached his blood and heart, requiring emergency surgery.
Brauner’s surgery saved his life but left deep, gaping wounds that failed to heal. He spent the next 10 years fighting the prison for medical care. As the official grievances he filed went nowhere, Brauner began to fear for his life. “I started seeing that they don’t treat nobody,” he says. “You get hurt, you get sick, or you can’t produce for them no more in their fields or in the hobby shop. … They put you on a ward on a bed and let you die.”
OLD TIMES THERE ARE NOT FORGOTTEN
Tucked into a bend of the Mississippi River, Angola is the largest maximum-security state prison in the country. It is also a working plantation bigger than Manhattan. Home to more than 6,250 male convicts and hundreds of “freepeople” (employees and their families), the penitentiary gets its name from the Angolan slaves who once worked its fields. Today, the cotton is picked and the sugar cane cut by crews of prisoners, who are mostly black, overseen by armed guards on horseback.
From 1995 to 2015, Angola’s warden was the controversial and larger-than-life Burl Cain. Under his reign, the prison received regular media attention, particularly during the “inmate rodeo” held eight weekends a year, where incarcerated men are tossed like rag dolls by charging bulls in a prisoner-built arena that can hold 10,000 cheering spectators. Cain opened the prison gates to film crews, reporters and curious tourists who wanted to visit the on-site golf course, museum and gift shop selling “Angola: A Gated Community” shirts. Evangelical Christians revered him for his work building chapels on Angola’s expansive grounds and bringing captive souls to Jesus.
Cain, who stepped down in 2015 amid revelations of suspect real estate dealings with relatives of prisoners, spent his career one step ahead of scandal: During his tenure, a journalist accused him of extortion, the FDA seized cases of expired evaporated milk that prisoners were labeling for resale, and prisoners brought suits alleging discrimination against non-Evangelicals. He always managed to avoid court, assisted by his deep family connections, charisma and the reputation he cultivated for ending Angola’s era as America’s bloodiest prison (though the violence receded long before he took the job).
Angola is also widely known for its on-site hospice, where dying men receive end-of-life care from fellow prisoners. The hospice is the subject of a feature-length documentary produced by Oprah and narrated by Forest Whitaker. Prisoners who die at Angola receive elaborate funerals, complete with a horse-drawn hearse, a handmade coffin and burial in one of two prison graveyards.
Yet, judging by the experience of Brauner and hundreds of other incarcerated men, the respect offered to the dead and dying at Angola deflects attention from a brutal reality: Death at Angola comes earlier than it should, and sickness and suffering are more prevalent than they need to be — all due to the miserable level of healthcare the State of Louisiana offers Angola’s prisoners.
DEATH ON THE INSTALLMENT PLAN
Desperate for better care, Brauner secretly recorded the details of his medical treatment, hoping to build a lawsuit against the prison and medical staff. “Day by day, I documented,” he says. “What date, what doctor came to see me, what he said, what he didn’t say, what he didn’t do. What the nurses are doing, what time they’re doing it, if I was left to lay there half the day before my dressings got changed.” He befriended other men in the nursing ward and began keeping records of their treatment as well. “I watched so many people die that didn’t need to die,” he says.
Brauner kept the logs hidden in his locker, and in 2012 showed them to Nick Trenticosta, a New Orleans-based attorney who was considering using Brauner as a witness in an unrelated death penalty appeal. Trenticosta looked around the nursing ward and saw open garbage containers, showers filled with mold and mildew, and tape covered in dead flies hanging over patients’ beds. He connected Brauner to several prisoners’ rights attorneys who began meeting with other Angola prisoners.
In May 2015, a group of incarcerated plaintiffs filed a class action lawsuit on behalf of the thousands of men held at Angola, alleging that the prison’s medical care violates the Constitution’s Eighth Amendment prohibition against “cruel and unusual punishment.” They are represented by attorneys from four firms — Advocacy Center, ACLU of Louisiana, Promise of Justice Initiative and Cohen Milstein Sellers & Toll PLLC — and are suing four defendants: Darrel Vannoy, who replaced Cain as head warden in late 2015; Stephanie Lamartiniere, assistant warden for health services; James LeBlanc, Louisiana’s secretary of corrections; and the state Department of Corrections (DOC) itself. The lawyers interviewed hundreds of men to build their case and documented one medical horror story after another.
Plaintiff Shannon Hurd, 41, was charged with first-degree robbery in 2003 for breaking into a family’s home and stealing $14, and was convicted by a non-unanimous jury. No one was harmed, but since Hurd had prior felonies, he received a mandatory sentence of life in prison without parole.
According to the complaint, at Angola, Hurd developed extreme pain in his side. He repeatedly requested medical attention starting in 2010, but his pain was dismissed as gas. Over the following five years, he developed numbness in his feet, legs and fingertips, lost his appetite, and dropped nearly 100 pounds. When he finally received a CT scan in 2015, he was diagnosed with stage 4 cancer in his kidneys and lungs — most likely a terminal condition.
Another plaintiff, Alton Adams, 53, suffers from peripheral artery disease, but allegedly was told the state could not afford the stent he needed to save his right leg. A blood clot formed that led to three consecutive amputations. According to the complaint, Adams sees the same issues developing in his left leg, but fears that if he pushes for care, he will face retaliation.
The Louisiana Department of Corrections, which runs the prison, did not respond to requests for comment by In These Times, citing ongoing litigation. In a 2015 media statement, the DOC said that despite challenges like the high numbers of older prisoners and those with chronic diseases, the prison “has provided appropriate, quality care.”
Sandy Netherland-Roberts, a nurse who ran the prison hospice from 2009 to 2011, maintains that Angola’s healthcare is comparable to care on the outside. “Does the system get backed up some? Absolutely. But if you’re in a charity system, even free people on the outside, do they not wait for several months to get an appointment if it’s non-emergent? Absolutely.”
Dr. Anjali Niyogi, who directs a transition clinic for the recently incarcerated in New Orleans and treats current Angola prisoners as a physician at University Medical Center, has a different perspective. “We do see a lot of delayed care coming out of Angola,” she tells In These Times. “People who probably should have been seen honestly, years or months earlier.”
SUSPECTED MALINGERERS
Angola has a documented history of substandard medical care. In the 1990s, prompted by a class action lawsuit, the Department of Justice conducted an investigation and reported to the court that Angola “fails to recognize, diagnose, treat or monitor the serious medical needs of inmates.” The prison and plaintiffs reached an agreement in 1998 that put Angola under a temporary federal monitor.
The current lawsuit points out that many of the medical practices described by the plaintiffs echo those condemned by the DOJ 25 years ago, including delays in care, underqualified staff and a “malingering” rule that effectively punishes people for requesting medical assistance.
According to the lawsuit and interviews conducted by In These Times, at Angola today, emergency medical technicians (EMTs) — not physicians, physician assistants or nurses — are the gatekeepers who determine which patients need urgent medical treatment and which should be sent back to their cells. EMTs receive between 140 and 1,111 hours of training, compared to the years required for medical degrees.
If the EMTs suspect a patient of malingering, or faking illness to get out of work, he may receive a disciplinary write-up, which can lead to extended solitary confinement. Clifford Doleman, who was incarcerated at Angola from 1994 to 2016 and worked as a prisoner orderly there, says that the ailing men he assisted were afraid to request medical care, thanks to a general assumption that prisoners were faking.
In a deposition in August, Angola Medical Director Randy Lavespere explained his biggest challenge was determining “who’s telling the truth.”
“A lot of them use the medical department for reasons not to go to work,” he said. “In Angola, they don’t necessarily want to get well.”
Plaintiffs say the EMT triage system and distrust of prisoners cause long delays in care. In a 2014 email entered as trial evidence, the LSU hospital stroke coordinator complained, “In the past month and a half I have had three inmates from Angola that presented with obvious stroke symptoms. All of them were out of the window [for treatment] because it either took them a while to get here or the medical staff at Angola did not think the inmate was having a stroke.”
Brauner says he’s seen the same thing happen to cancer patients. “They keep complaining about the same thing [but] the EMTs will just say, ‘Well you got a stomach virus, give him Pepto-Bismol, just give him something and get him out of here.’ If you go there too much, they’ll write you up for malingering. So then all of a sudden they decide to finally send him out, well, he’s already got Stage 3 cancer. Because they procrastinated and procrastinated, this guy’s dying.”
And people do die at Angola, at extremely high rates. In 2015, there were 58 deaths — more than one a week. That mortality rate — 923 deaths per 100,000 prisoners — dwarfs the nationwide average in state prisons, which was 274 deaths per 100,000 in 2013 (the most recent year data was available).
One factor is the large proportion of Angola’s prisoners serving life sentences — more than 65 percent — thanks to Louisiana’s draconian sentencing laws, like the one that sent Shannon Hurd to prison for life over $14. Twenty-five percent of Angola’s prisoners are 55 or older, compared to just 10 percent in state and federal prisons nationwide.
But it’s not just old men who are dying. Last year, mortality rates at Angola were higher than the 2013 national averages for prisoners in every single age group over 25.
A LOW PRICE ON HUMAN LIFE
Despite the complex healthcare needs of its aging population, Angola spends far below average on medical care. According to numbers provided to In These Times by the Louisiana DOC, a total of $18.82 million was spent on healthcare at Angola in 2015, or just under $3,000 per person. The Pew Research Center calculated that in 2011, the national per capita average for state prisons was $6,047.
Angola’s low medical spending stems in part from Louisiana’s ballooning budget deficit. This year the state cut funding for public colleges, schools and healthcare providers, as well as prisons.
In 2010, Louisiana spent less incarcerating each prisoner than all but three other states, and per-prisoner spending has only dropped since. This year the state lowered the daily per-prisoner reimbursement rate from $31.51 to $24.39 at two privately run facilities. As a result, the contract was renegotiated to convert them from prisons to jails, which means the facilities no longer need to provide medical services. People with chronic conditions are being transferred to state-run facilities.
Frustrated with budget cutbacks, in March Louisiana Corrections Secretary James LeBlanc (a defendant in the lawsuit) told the Advocate that lack of funds was affecting the care of incarcerated men and women. “We can’t medicate them, we can’t house them, we can’t feed them — and those are constitutional issues.”
Angola’s medical costs increased in 2013 and 2014 when the state privatized nine LSU hospitals in no-bid contracts under former Gov. Bobby Jindal. In the hospital realignment, the state closed Earl K. Long Medical Center in Baton Rouge, which had handled the vast majority of Angola’s hospital visits. Angola now sends emergency cases to two area hospitals, and patients needing ongoing treatment (as well as some emergencies) are transported to University Medical Center in New Orleans, over two hours away.
Angola recoups some money by charging co-payments, a common practice in U.S. prisons and jails. Individuals are charged $3 for routine sick calls and $6 for emergency calls — regardless of whether the EMT sends them on to see a doctor. Prescriptions cost $2. According to numbers provided by the DOC, Angola billed more than $192,000 in co-payments over three years.
The men held at Angola make as little as four cents an hour for grueling fieldwork, meaning it could take 150 hours to pay off a single $6 co-pay for an emergency assessment. And while the prison is constitutionally obligated to care for patients who can’t afford the co-pay, that debt doesn’t disappear. “The bills stack up,” says Francis Brauner. “If you ever do get money, they take all that money to pay toward your medical bill. And if you don’t, and you leave prison, it follows you.”
DOCTORS WITHOUT LICENSES
Attracting doctors to work in Louisiana prisons can be a challenge. The pay, although six figures, is lower than in private practice, and some physicians are reluctant to come to rural areas or to work with a high-risk, stigmatized population.
The state DOC has a solution to this problem: It hires doctors with suspended licenses. The Louisiana Medical Board allows physicians whose medical licenses have been suspended for legal or ethical violations to practice in prisons, a policy that is strongly opposed by the two major national professional organizations of correctional physicians, the National Commission on Correctional Health Care and the Society of Correctional Physicians.
Since the beginning of 2011, 14 physicians have been employed by Angola. Twelve came to Angola after receiving disciplinary sanctions from the state medical board for misconduct. Dr. Hal MacMurdo, who was hired as a physician in September 2010 and is now assistant medical director, had a suspended license from September 2010 to September 2015 for allegedly drinking on the job. The license of another Angola physician, Dr. Paul Toce, is on indefinite probation for “professional sexual misconduct.” Current Medical Director Dr. Randy Lavespere served a two-year prison sentence and had his license suspended from October 2009 to October 2014 for purchasing crystal meth with the intent to distribute in 2006 (he was hired at Angola in September 2010). The state medical board noted that Lavespere was diagnosed with amphetamine, cocaine and cannabis dependence, in addition to adjustment disorder and personality disorder with antisocial, narcissistic and avoidant features.
Dr. Tobe Momah, whose record is clear of ethical violations, worked at Angola in 2011 and 2012. He says he felt called to Angola after hearing Burl Cain speak at a church, but admits that his colleagues with suspended licenses didn’t necessarily share a “mission-minded” philosophy. “It doesn’t mean they were bad,” he told In These Times. “It just means their vision, motive, philosophy was different. Some of them were just like, ‘I just want to get this over with and get back to my life.’ ”
Dr. Raman Singh, medical director of the state DOC (and former Angola medical director), defended the practice of hiring unlicensed physicians in a 2012 interview with the Times-Picayune. “I can’t find a doctor at all for six months, and that creates a huge liability for the unit and for the institution,” he said. “When I was new, I was told that ‘We just need a body in that job.’ Sometimes it’s so desperate a situation, you just need a body in the job.”
Correctional physicians can reasonably handle caseloads of 600 to 800, according to a healthcare evaluation of Angola conducted by medical examiners for the lawsuit. At Angola, three physicians and one nurse practitioner are responsible for almost 1,600 patients each.
DELIBERATE INDIFFERENCE
Some prison staff describe an adversarial relationship with prisoners they believe are overly eager to sue them. “The offenders taught me everything I needed to know about covering your behind,” says former hospice manager Sandy Netherland-Roberts. “They will find every way possible to burn you. They have nothing but time to figure out a way.”
In fact, it is very difficult to file successful lawsuits from prison. The federal Prison Litigation Reform Act (PLRA), passed in 1996, places tight restrictions on incarcerated plaintiffs in a supposed effort to limit frivolous litigation. Plaintiffs must first exhaust the prison grievance process, and PLRA caps the fees that prisoners’ attorneys can recoup from the prison if their client wins.
These barriers succeed in blocking litigation: Despite thousands of health-related grievances filed each year, the Louisiana DOC faced just 40 lawsuits related to physical and mental healthcare in 2015.
Even when incarcerated people manage to get their cases heard in court, the deck remains stacked against them. Plaintiffs have to prove deliberate indifference on the part of the prison. One federal judge used a colorful metaphor to define how high a bar this is: If prison officials “place a prisoner in a cell that has a cobra, but they do not know that there is a cobra there, or even that there is a high probability that there is a cobra there, they are not guilty of deliberate indifference — even if they should have known about the risk.” When Francis Brauner filed a lawsuit against Angola, it was thrown out on the grounds that he could not demonstrate deliberate indifference.
Attorney Nick Trenticosta believes the judicial system shouldn’t treat prisoners’ claims with extra suspicion. “The majority of prisoners are honest people,” he says. “They have health needs. They present those health needs and unfortunately, it appears they are met with skepticism.”
Mercedes Montagnes, lead attorney in the class action suit, says PLRA’s restrictions on prisoner litigation are similar to the concept of allowing physicians with suspended licenses to work in prisons: Both are double standards that place a lower value on incarcerated lives. “There are two ways to look at prisoners,” she says. “That they deserve less good care, which I think is pretty awful, or they are the most vulnerable patients a person can have. The most, bar none.”
Others feel conflicted about the state’s obligation to cover expensive medical treatment for convicted felons. In early 2016, state Sen. Yvonne Dorsey-Colomb questioned the expensive medical treatment the state was providing for Derrick Todd Lee, a death row prisoner convicted of two murders and linked to five others, including the brutal murder of Dorsey-Colomb’s stepdaughter. “He’s still here, and he can still go get healthcare when all the victims are dead by his hands,” she told the Advocate.
Yet if the state cannot afford the care it is constitutionally obligated to provide, perhaps it is incarcerating too many people — a point the U.S. Supreme Court made in 2011 when it mandated the reduction of California’s prison population in Brown v. Plata. In that case, the Court determined that if a prison “deprives prisoners of basic sustenance, including adequate medical care,” the courts have a responsibility to intervene, including through “orders limiting a prison’s population.”
Incarcerated people are uniquely at the mercy of the state. They are uninsured, have to jump through hoops to see a doctor and are unable to seek a second opinion when told there is nothing wrong.
U.S. prisoners serve sentences unimaginable in the rest of the developed world, but nobody is sentenced to premature death by medical neglect. Francis Brauner recalls telling doctors, “I’m not sentenced to death. And that’s the bottom line.” But for too many, getting sick in Angola is a death sentence.
When the lawsuit was announced in 2015, the lead plaintiff was 81-year-old Joseph Lewis, who allegedly spent three years submitting sick call requests for chronic throat pain without receiving anything stronger than Q-Tussin spray. Finally, after he was visited by attorneys, prison officials took him to a hospital, where the doctor recommended an immediate biopsy. When Lewis received the test — more than two months later, according to the lawsuit — he learned he had throat cancer. He died within eight months of related complications.
The plaintiffs in Angola think their unnecessary suffering is a form of cruel and unusual punishment, just as the Supreme Court ruled of California’s prison medical care in 2011. According to the complaint, men at Angola suffer hernias for years, develop life-threatening infections, or go blind from glaucoma. The medical examiners who investigated Angola for the lawsuit concluded that, in their collective 60 years of correctional medicine experience, “Louisiana State Penitentiary’s delivery of medical care is one of the worst we have ever reviewed.”
As of August 31, the DOC had billed $599,877 fighting the suit, which is scheduled to go to trial in May 2017. Meanwhile, according to the plaintiffs, prison officials have “attempted to paper over the problems identified in this lawsuit by transferring many severely disabled inmates” to Elayn Hunt Correctional Center, another state facility.
Mercedes Montagnes said her team’s goal is to bring healthcare to an adequate level for everyone at Angola. If the plaintiffs demonstrate a constitutional violation, the court can appoint a federal monitor to ensure that conditions improve.
Francis Brauner was released on parole in 2015, after serving 17 years. As a free person, he is ineligible to be a named plaintiff in the class action suit. At press time, he was still awaiting surgery to close his wounds. 
This reporting was made possible by a grant from the Leonard C. Goodman Institute for Investigative Reporting.




