11 Statistics That Show Racism Is Entrenched in Our Healthcare System
Covid-19 is disproportionately harming Black Americans. This is not an exception, but the rule.
Dayton Martindale
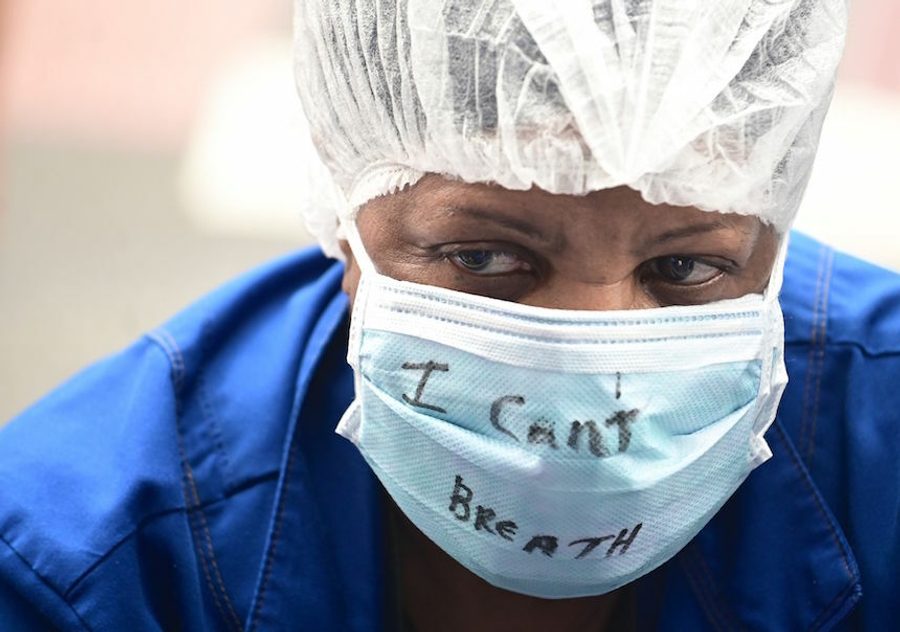
It has been widely reported by now that Covid-19 has raged through communities of color with particular violence. Nearly one in four Covid-related deaths have been Black Americans, more than twice the rate of white Covid-19 deaths; 31% of Black Americans know someone who has died, compared to 9% of whites.
This stark divide is nothing new. At every level, this country has long failed the health of its most vulnerable residents. Black Americans face worse air pollution and greater food insecurity, are less likely to be insured, and in many cases are less likely to be prescribed or referred to necessary treatment. The constant stresses of racism increases allostatic load, a measure of wear and tear on the body that increases likelihood of high blood pressure, diabetes-related deaths and other health issues. And given the history of abuse by doctors and researchers, there is a justified lack of trust in the medical establishment.
All of this means that Black Americans face disproportionate harm from nearly every major medical issue — the coronavirus’s impact is not an exception, but the rule. The following numbers offer a snapshot of these harms and their causes, evidence that radical transformations in the healthcare system are needed to truly make Black lives matter.
- 14% of second-year med students (wrongly) believe Black people have less sensitive nerve endings than white people
- 47% of the time, U.S. physicians underestimate the pain levels of Black patients, compared to 33.5% for white patients
- 13% of U.S. residents are Black
- 5% of U.S. physicians are Black
- 19% reduction in the Black-white disparity in men’s cardiovascular mortality could be achieved if more doctors were Black
- 25% of Black Americans live in an area with a shortage of primary care physicians
- 243% more often than white women, Black women die from pregnancy or childbirth
- 16 more minutes, on average, are spent in the ER waiting room by a Black person, compared with a white person
- 200,000,000 patients have been screened by medical centers using commercial algorithms to predict the need for follow-up care
- 18% of those automatically referred for extra care by one such algorithm were Black
- 47% of the patients who should have been flagged for extra care were Black, which the algorithm missed due to racial bias
Dayton Martindale is a freelance writer and former associate editor at In These Times. His work has also appeared in Boston Review, Earth Island Journal, Harbinger and The Next System Project. Follow him on Twitter: @DaytonRMartind.








